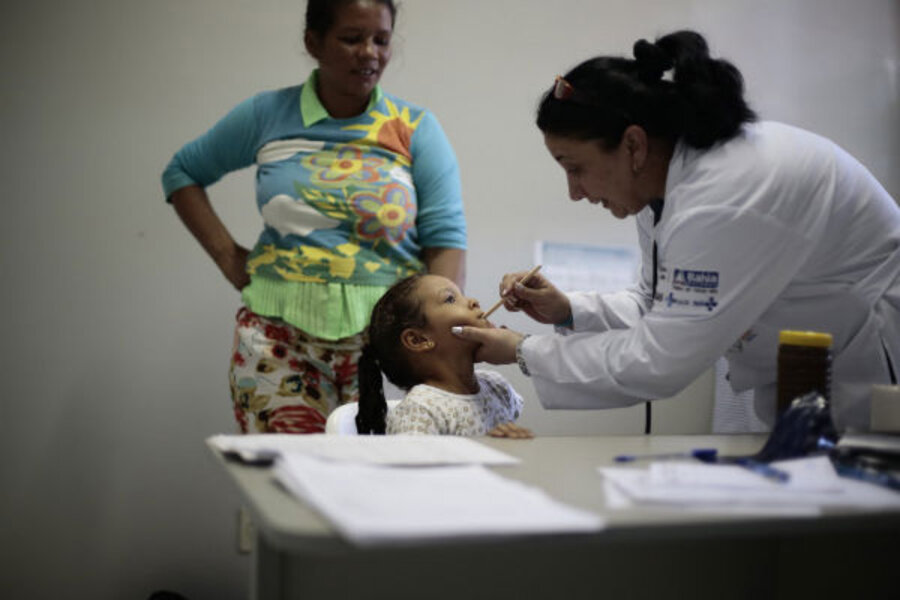
Trading wellness tips, Brazil's community workers plug primary health gaps
Loading...
| São Paulo, Brazil
Marcia Cristina Bonfante and Adriana Siqueira Lima live in the same neighborhood in western São Paulo and have daughters around the same age. But when Ms. Bonfante drops by her neighbor's house, it's more than a simple social call. As a community health worker, Bonfante makes hundreds of such calls every month.
Bonfante and four other government-paid community workers service over 2,000 families in their neighborhood of Coahab Raposo Tavares. They inquire about the family, recent health concerns, and share tips on hazards such as stagnant water that might attract dengue-spreading mosquitoes.
Today Bonfante asks Ms. Lima about her recently broken toe and checks if anyone in the home has had a cough for more than three weeks – a possible sign of tuberculosis, which has been on the rise in the area.
Last summer when protests against poor public services spread across Brazilian cities, one recurring complaint was over access to quality health care. Such complaints weren't new – in 2011, almost 78 percent of Brazilians reported dissatisfaction with public hospitals, according to a Latinobarómetro poll – but watching the government spend billions of dollars on World Cup-related projects, rather than healthcare, stirred popular frustration.
Brazil’s 1988 constitution guarantees universal health care. And the country has made progress on public health indicators, cutting the prevalence of communicable diseases such as HIV/AIDS, offering universal access to treatment, and reducing infant mortality by two-thirds between 1990 and 2011. (The mortality rate for children under 5 is now 15.6 per thousand.) But access to quality care is quite limited, with significant variation not only among regions but also often among different neighborhoods of the same city.
According to a 2002 study by the National Institute of Health, the poorest Brazilians have “less access to health insurance, greater need for medical care, and lower consumption of such services.” In 2013, the United Nations found that the richest 20 percent of Brazil’s population are twice as likely to receive prenatal care as the poorest 20 percent of the country.
Income inequality and health
“Income inequality is a core characteristic of Brazil,” says Alexandre Chiavegatto Filho, assistant professor at the University of São Paulo who studies the intersection of income inequality and health. When inequality in a neighborhood or city is high, there are also higher rates of mortality.
The community health worker model was first launched in the late 1980s in northeastern Brazil. It reached Bonfante's neighborhood in 2002, which is when she joined up. The program, which consists of multiple teams made up of one doctor, nurse, and nurse assistant, along with about five community health workers, expanded across the country when it was shown to decrease infant and maternal mortality rates in participating communities.
The idea is for patients and doctors to connect more regularly than via sporadic visits to a clinic. It focuses on preventative care and creates a link to basic health services for Brazilians who are far removed or financially excluded from care.
Lima lives more than 40 minutes by foot from the closest primary care provider, the UBS Jardin Boa Vista. The clinic opened in 1996 and has roughly 100 people on staff, including medical professionals. It is the only public clinic serving a densely populated area of nearly 20,000 people.
“Before the [community] health program, primary care meant clinical consultations,” says Dr. Janos Valery Gyuricza, who works at the Boa Vista clinic. Now that community workers check in with patients in their homes, “we can see social issues as health [issues].”
Cross-town trek
But there’s still plenty of room for improvement. Lima broke her toe two months ago – on a Sunday. The Boa Vista clinic was closed, which meant a long cross-town multiple-bus trip to find an emergency room.
Non-emergency treatment can also be tricky. If Lima wants a mammogram this year, she could wait more than four months to get an appointment, Bonfante says. And despite Bonfante’s 12 years working as a paid community health liaison, she has never gone through a training program or received formal medical instruction.
As Bonfante walks out of the squeaky gate of Lima’s apartment complex, a young woman stops her on the street to ask how she can schedule a prenatal checkup. This is what Bonfante does best: consult and guide those in need of health services.
Unfortunately, this woman doesn’t live within the Boa Vista clinic's neighborhood limits, Bonfante says. The expectant mother will have to find another place to go.
Whitney Eulich reported from Brazil as a fellow with the International Reporting Project (IRP)