Why heroin is spreading in America's suburbs
Loading...
| newburyport, mass.
Ana was a good student in middle school. She got above-average grades, seemed poised and self-possessed, and, like many of her friends in her charming coastal town north of Boston, was on a probable path to college. Then, during her freshman year in high school, she decided to experiment with drugs and alcohol.
One night she got very drunk with some friends and loved it. She says it made her feel like "the person she wanted to be." Before long she was also smoking marijuana. Soon after, a friend gave her some prescription painkiller pills to try, which Ana (not her real name) says made her feel even better than the alcohol.
She started buying the pills illicitly – often spending several hundred dollars a day. She stole to support her habit, but it wasn't enough. Then her friend asked her: Why not try heroin, since it's so much cheaper? Ana was shocked. Heroin, after all, was for "real" drug addicts.
But by that time her dependence on the painkillers had become more than she could resist. She bought the heroin, snorting the powder at first. But within six days she was injecting herself with a needle – becoming the archetype of a classic heroin addict.
Ana's anguished journey from conscientious student to heroin user is one confronting many young people in suburbs across the country. From Los Angeles to Long Island, Chicago to New Orleans, parents and police are struggling with a rise in heroin use in suburban neighborhoods more often concerned with SAT scores and the length of lines at Starbucks.
The rise is being driven by a large supply of cheap heroin in purer concentrations that can be inhaled or smoked, which often removes the stigma associated with injecting it with a needle. But much of the increase among suburban teens, as well as a growing number of adults, has also coincided with a sharp rise in the use of prescription painkiller pills, which medical experts say are essentially identical to heroin. These painkillers, or opioids, are prescribed for things such as sports injuries, dental procedures, or chronic back pain. Yet in a disturbing number of cases, experts say, they are leading to overdependence and often to addiction to the pills themselves, which can then lead to heroin use.
The latest rise in heroin abuse was made more visible by the recent overdose death of actor Philip Seymour Hoffman. But use of the drug has been growing steadily across many levels of society for at least the past five years. And unlike the heroin surge in the 1970s, the current use of opiates is far more concentrated among suburban and rural whites than among African-American and Latino communities.
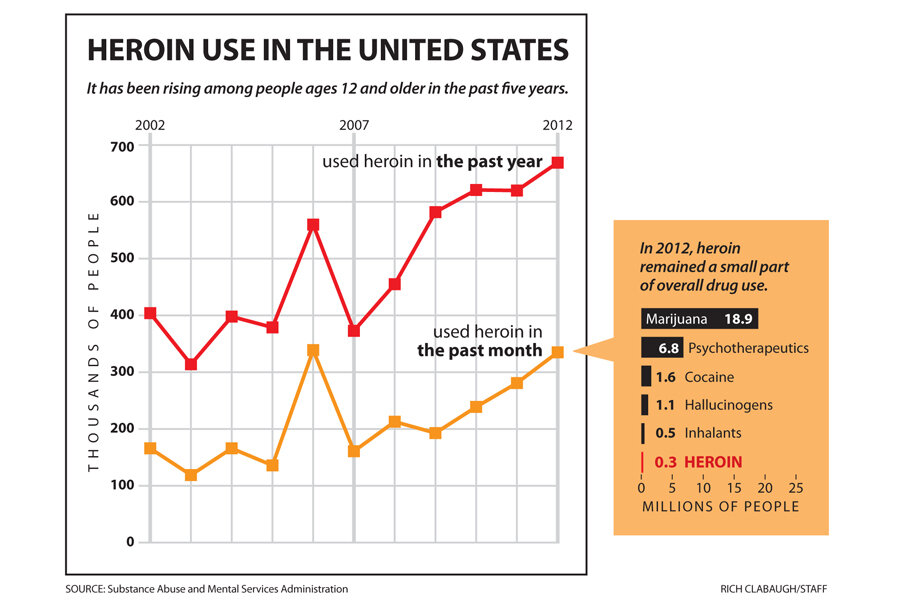
In Vermont, Gov. Peter Shumlin in January devoted his entire State of the State message to the heroin and opiate addiction crisis engulfing his state. [Editor's note: The original story solely mentioned heroin.] In Massachusetts, law enforcement authorities recently reported that 185 people have died of heroin overdoses in just the past four months – which didn't include numbers from the state's three largest cities. Nationwide, according to the federal Substance Abuse and Mental Health Services Administration (SAMHSA), heroin use among persons age 12 and older nearly doubled between 2007 and 2012.
"The perception [used to be] that heroin was mostly an urban problem," says Anthony Pettigrew, an agent with the Drug Enforcement Administration (DEA) based in New England. "But now there are no borders, there are no demographic or geographic areas ... that are immune from heroin."
• • •
Donna Holaday looks out the window of her city hall office in Newburyport, an affluent coastal city 37 miles north of Boston. Ms. Holaday has been mayor of the town the past four years and was recently reelected. Over that time, she has seen her share of municipal concerns come across her busy desk. But few have been as worrying as the growing use of heroin in her idyllic community.
Although she knew of the drug's presence in the city, Holaday says that it wasn't until police reports started surfacing and concerned residents began showing up in her office that she understood the depth of the problem and the emotional anguish it was causing.
"I had a mother sitting in my office crying, telling me her story about how she pulled her son out of a trailer, just over the border in New Hampshire, and [how] he would have died [if she hadn't intervened]," she says.
Other local parents told her about finding needles and syringes in the leafy playgrounds where their children romped. Addicts were seen "shooting up" on the city's Clipper City Rail Trail, a scenic biking and jogging path. Newburyport Police Marshal Thomas Howard says his department has responded to more than a dozen heroin overdoses in the past six months. Without the use of Narcan, an overdose reversal drug, he says the number of deaths in the area "would be skyrocketing."
Normally, Newburyport isn't the kind of town you'd expect to have any heroin footprint at all. It is one of those communities that seems to have everything: beauty, wealth, a vibrant arts culture, and an enviable location. Straddling the banks of the Merrimack River and its outlet to the Atlantic Ocean, Newburyport has a storied seafaring heritage that is visible at every salt-scented turn.
Its harbor once bustled with clipper ships from around the world. The city's High Street is a showcase of imposing Federal-style homes that trace their lineage to sea captains and speculators who plied the waters of the West Indies, trading molasses for rum in the 1700s. These same homes, once maintained by black and native American slaves, later became a means of escape as part of the Underground Railroad.
Now this city is trying to end a different kind of slavery. Mr. Pettigrew, of the DEA, lives in Newburyport. As a member of the agency's regional office, he and his fellow agents track where the drugs flowing into New England are coming from – a trail that usually leads to cartels in Colombia and Mexico.
While heroin has always been available in the region, what's changed recently is the purity of the drugs on the street. Pettigrew notes that the heroin that addicts used to shoot up with was 2 or 3 percent pure. Today, the street purity of the drug can be as high as 80 percent.
That potency helps explain both the drug's wider appeal and its new danger. Heroin once had to be injected for users to get the high they were looking to achieve, but it is now concentrated enough that they can smoke or snort it to get a similar effect – methods that make heroin easier for people like Ana to use it without feeling like a junkie. The higher purity is also more likely to trigger an overdose for those who do inject it.
"Like everything else, you're trying to sell your product, so [dealers are] trying to pitch it as a more potent drug for you to take and get high off of," says Mr. Howard, the police marshal.
• • •
Stronger heroin is only one reason behind the nation's growing addiction problem. The other – and more prevalent cause, say police and medical experts – is the nation's pill culture.
Ana's route to addiction is a familiar one, according to addicts: a progression from alcohol to marijuana to painkillers to heroin. There are variations on that theme: a sports injury and a prescription for opioids that goes on far longer than it should; a peek inside the family medicine cabinet to find a trove of prescription pills – such as Percocet, OxyContin, Vicodin, codeine – that can be used as recreational drugs.
Often the introduction comes through friends who want to share a high they have discovered. Or it happens at a college party where a variety of drugs are being offered.
Regardless of how it starts, it usually takes the same precipitous route. Once hooked, users look for doctors who will sell them prescription drugs and, failing that, turn desperately to the street, where the price can be as high as $80 for a single pill. When that becomes too expensive, users often resort to the drug that produces the same kind of high that painkillers do but is far cheaper: heroin.
Yet opioids are dangerous in their own right. According to a series of papers by the Centers for Disease Control and Prevention (CDC) in Atlanta:
•More than 12 million Americans reported using prescription painkillers in 2010 without a prescription or just for the high that they cause.
•Nearly 3 out of 4 drug overdose deaths are now caused by prescription painkillers. In 2008, some 14,800 deaths were attributed to the pills – "more than cocaine and heroin combined."
•More than 475,000 emergency room visits were directly linked to prescription painkiller misuse or abuse in 2009, roughly double the number of five years earlier.
The global production of oxycodone, marketed as OxyContin in the United States, increased from two tons in 1990 to 135 tons in 2009. More than two-thirds of that supply was manufactured in the US, which, according to the United Nations Office on Drugs and Crime, increases the risk of its subsequent overprescription and diversion into illicit channels.
Experts trace the rise of painkiller misuse in the US to 1996. That's when the pharmaceutical company Purdue Pharma introduced OxyContin, a narcotic and derivative of opium. Andrew Kolodny, chief medical officer of Phoenix House, a national nonprofit treatment agency, describes OxyContin as essentially a "heroin pill." It was made of oxycodone, a narcotic used to treat pain at the end of life. But the new pill would allow the company to reach a much wider audience.
"[Purdue] wanted a product that would be prescribed for common, moderately painful chronic conditions," says Dr. Kolodny, who is also president of Physicians for Responsible Opioid Prescribing, an advocacy group.
At first, the medical community balked. Using opioids for chronic problems seemed too risky given the nature of the pills' highly addictive properties. But Purdue Pharma launched an aggressive marketing campaign arguing that it was a compassionate way to treat patients and, because of its extended-release characteristics, would be less prone to abuse.
But before long, numerous cases of addiction to the painkillers began to surface. In 2007, Purdue Pharma pleaded guilty in federal court to misleading doctors and the public about OxyContin's risks and paid a $600 million penalty.
Kolodny says that the overprescribing of painkillers has now led to an "epidemic" of addictions, both among pain patients and recreational users.
Yet others are far less dire in their assessment. Daniel Carr, a professor in the department of public health and community medicine at Tufts University School of Medicine in Medford, Mass., notes that about 80 million postoperative patients receive opioids every year without necessarily becoming addicted to them. He says it has been standard procedure to administer painkillers to patients for the past 40 years. He calls pain a "big public health problem."
"The average person does not experience euphoria, just pain relief," says Dr. Carr. But a tiny minority, he adds, try to manipulate the process and get more drugs than they're supposed to.
Yet critics argue that prescribing painkillers to postoperative patients is different from prescribing them to teenagers who sustain football injuries or who just had their wisdom teeth removed. Kolodny says doctors have been taught to put patients on extended-release opioids that can be taken two or three times a day. "So what happens is that within a week your body starts to become dependent on the medicine and it becomes very difficult to get off it," he says.
And once a person becomes addicted to painkillers, it isn't a long journey to heroin – itself a derivative of morphine developed in the late 1800s as a painkiller. Joseph Gfroerer of SAMHSA co-wrote a recent study that found that, of those who had tried heroin, about 80 percent had previously used painkillers without a prescription.
• • •
Michael Wilson epitomizes how seamless the move between heroin and painkillers can be. In his teen years, Mr. Wilson says he would try anything once. If he liked it, he would keep doing it. That experimental fervor led to addiction, homelessness, and prison.
Wilson was about 17 years old when a friend introduced him to heroin. "I tried it and fell in love with it," he says. "It became the most dominant relationship in my drug life."
Even though he was regularly snorting heroin, it was OxyContin pills that he became addicted to. But he and his drug-using friends still didn't think of themselves as addicts: They rationalized that they were just doing the heroin until they could get hold of their preferred prescription pills. They refused to think of themselves as "junkies," whom they sneered at. "It was like a group delusion," says Wilson.
Waking up from that delusion came about after many hard trials of alienation from his family, bouts of time in jail, detox, and rehabilitation, and eventually the move from snorting heroin to shooting it. Finally, Wilson developed a deep desire to spare his son the shame of what his drug addiction could mean for his future.
Today he is not only free of drugs but has started a nonprofit family support group and referral service in Beverly, Mass., the Renewed Hope Project, to help others overcome the ordeals of addiction.
For most trying to reclaim their lives, the road to recovery can be a constant challenge, both for the addicts and their families.
Nancy's journey with her daughter Lauren began in middle school. Lauren (not her real name) started by drinking alcohol and experimenting with marijuana. By her freshman year in high school, she had stopped participating in sports and was nodding off at the dinner table. By her sophomore year, she was taking "a lot of pills and a lot of cocaine."
She also had an abusive boyfriend who supplied her with drugs and convinced her to break into a local gym to steal from the lockers. The once close family was in a perpetual state of chaos. Nancy (not her real name) looked at programs out of state, anything to get Lauren away from her deteriorating lifestyle. "We found her just slipping away," she says.
The family decided to spend the money they had saved for remodeling their kitchen – some $80,000 – to send Lauren to a treatment facility in Montana. It was during a visit there, three months into the program, that the parents found out about Lauren's heroin use. They had assumed it was just pills and alcohol.
"I had to get up and leave the meeting," says Nancy. "I remember turning on her and saying, 'I hate these drugs. I hate what they do to you. I hate that you sell your family and your soul and we're like way over there – we're like thrown away for these drugs.' "
Those feelings aren't unusual. Treatment experts say families often experience extreme emotions: They feel both anguish for the struggling addict and a sense of isolation because of the judgments they often have to endure from extended family and friends.
When Lauren returned from the treatment program in Montana, all went well for a while, but old friends, old haunts, and old habits proved too much. She was soon shooting heroin again, stealing from the family-owned business, and trading sex for drugs. It would take more trials and more determination for Nancy and her husband to decide that Lauren would have to want to be free of the addiction herself. Talking to other parents with drug-addicted children was the first step of recovery for the family. "Finding a support group was a lifesaver for me, because people talk the same language that I talk," says Nancy.
Within the security of these support groups, she says, addicts feel free to share their stories, and unlike when they were using drugs, don't blame everyone else for their troubles.
"They always say, 'it wasn't [my] parents, it was me, something lacking in me, something that could never be filled. I wanted the latest craze, the fast music, the best iPod or whatever. I had to have the newest iPhone and sneakers.' But they're like, 'it was me.' "
Treatment providers agree that only by approaching the opioid drug problem systematically can there be meaningful progress – be it in prevention, education, or rehabilitation. And many believe the education process has to begin early – well before high school or middle school, perhaps as early as primary school.
"You have to talk to your kids as soon as [they can] understand the harm in taking drugs," says DEA agent Pettigrew. "I try to tell kids that I talk to that there will be a time that someone is going to offer you drugs. Chances are it's not going to be a stranger; it's going to be a friend, a teammate, a classmate. And you need to think ahead of time what you're going to say when that happens."
Others say that the education process should extend to the medical community. Kolodny argues that doctors, dentists, and nurses all need to know more about the dangers of painkillers and be more cautious in prescribing them, particularly with more powerful painkillers on the horizon.
Len Paulozzi, an epidemiologist at the CDC, agrees, saying that doctors in the US could learn from their counterparts in Britain and Scandinavian countries, where they prescribe far fewer opioids. But getting many in the US medical community to change practices won't be easy.
"Some prescribers are not going to take the training if it's optional," says Dr. Paulozzi. "Some may take the training if they have to, but it's not going to change their behavior. So we have to figure out a way to get your typical primary care doctor in communities across the country to have a better sense of the risks of [opioids] and a more real picture of the potential benefits."
Charles Faupel, a professor emeritus at Auburn University in Alabama and coauthor of "The Sociology of American Drug Use," points to another answer. He notes that the desire to alter consciousness is very strong in society. He'd like to see more spiritual grounding among young people.
"I think there needs to be a spiritual component to [education], but that's a very difficult thing to do in our day," says Dr. Faupel. "But I think that's an incredibly important missing element in kids' lives today."
For his part, Wilson believes in the "there is a solution" ethos that is a core part of the recovery group Alcoholics Anonymous. He doesn't accept the popular notion that addiction has to be a lifelong verdict.
"There's a solution for addicts, which is, if they want to change, they can," he says. "There's a solution for families, which is even if their loved one doesn't want to change, the family can. I just love that phrase, 'there is a solution,' because it implies that you can fix this. Not that you can fix someone else, but if you want to change, you can, you can be recovered...."
Ana is well on the road to recovery, too. She has been drug-free for several years now and is working at a treatment center north of Boston. "I used to think that alcohol made me [feel more like] myself," she says. "And then I realized that it just took me so much further away from who I really was and the person that I am today – and I love that person. So I think that surrounding myself with people that love me and saw me for who I was when I didn't was essential."